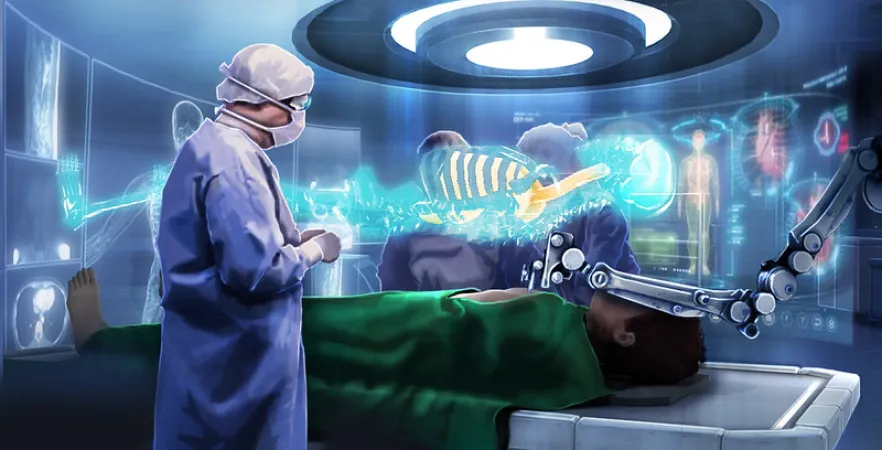
Looking into the future of medicine
What is the future of innovation in science and technology? What impact will it have on society?
These two questions underpin Curiosity on Stage, Ingenium’s thought leadership series on contemporary issues of global importance. Each event — staged at the Canada Science and Technology Museum in Ottawa — brings together leaders from private industry, academia, and government to discuss scientific and technological issues that are topical, divisive, and important to Canadians.
As we usher in a new decade, the medical industry is innovating at an incredible pace — producing technologies that will impact individuals and Canadian society as a whole. At a Curiosity on Stage event last fall, we asked, “What is the future of medicine?”
To discuss this question, we brought in two experts. Our first expert, Dr. Frank Rybicki, MD, PhD, is the Vice Chair of Operations and Quality at the University of Cincinnati’s College of Medicine, and the Director of Medical Affairs at Imagia, a leading healthcare AI company that unites healthcare expertise and advanced artificial intelligence technology to improve patient outcomes by enabling medical institutions to access and utilize healthcare data. Eric Ward, our second expert, is the Senior Director of Foresight at Policy Horizons Canada, the Government of Canada’s foresight organization, with a mandate to help the government develop future-oriented policies and programs that are more robust and resilient in the face of disruptive change.
Following the event, these experts spoke to the Ingenium Channel to share their insights about the future of medicine and health.

Ingenium Channel (IC): What is the most exciting development in medical research / biotechnology that you’ve seen recently?
Dr. Frank Rybicki (FR): Right now, the deployment of learning algorithms and computer based learning is the most important technology in medicine. No matter how hard we try, doctors do not have the mental bandwidth to analyze and identify links to diseases and cures as efficiently as computers. People and computers need to work synergistically.
Eric Ward (EW): I am very excited by some of the work that is being done, including in Canada, to design yeast, algae, and other microorganisms that produce valuable substances such as pharmaceuticals and fuels. Nature shows us that it is possible to create a huge variety of molecules at ambient temperatures using solar or chemical energy and circular flows of resources.
I am also fascinated by health advances such as a small, functioning 3D printed heart, 3D printed tumors that can be used to test therapies, chip-based optical sensors that detect cancer biomarkers in urine, and CRISPR gene biosensor platforms — the size of a credit-card — that connect to a smartphone to help spot diseases.
IC: Are there any recent developments in medical research / biotechnology that you find concerning? How can we make sure risks are managed?
FR: The ultimate goal is to preserve patient data privacy and educate the public that data, when used responsibly, leads to clinical insights that will improve patient outcomes and benefit patient care. The work that we are doing at Imagia is purpose-designed to solve the privacy issues that impede most health data-related innovation. We do this by enabling clinical researchers to learn from distributed patient data within our EVIDENS platform through federated learning. This approach allows us to gain insights while data remains in each institution, preserving the ability to scale up traditional discovery processes, and ensure privacy.
EW: I think that people are right to be concerned about “CRISPR babies” — the world’s first genetically-edited babies — and especially about genome edits that would be inherited by future generations. I personally do not feel as concerned about non-heritable genome edits to address a specific genetic disease from which an individual is suffering. One way of mitigating risks is to ensure that we are taking as many sources of knowledge as possible into account, including Indigenous worldviews.

Genetic engineering, like any other technology, has the power to be a positive or negative force in society.
IC: What are some major barriers to the implementation of medically disruptive technologies, the sort of discoveries that displace an established technology and shake up the industry?
FR: Trust. Change happens at the pace of trust. The public needs to understand that the overwhelming majority of healthcare providers understand the gravity of using medical data "for good.” However, no system is perfect. Imagia provides next-generation systems to ensure data governance which helps us gain critical trust with partners and patients.
EW: Cost could be a barrier, at least initially, but not necessarily because the therapy or device itself is expensive to produce. Instead, it might be hard to negotiate with innovators regarding the price assigned to patented breakthrough technologies. I’m thinking here about breakthroughs that could cure a disease outright rather than generating an income stream from long treatments with medication.
Limits to social acceptance could also slow some innovations, particularly with gene editing or human augmentations. That could be a good thing in some cases, if it arises from thoughtful consideration of risks and uncertainties. But there is also the potential for moral panics and misinformation to clutter the debate about new therapies.
It also takes time for regulations to adjust to innovations that don’t fit into previous categories. I don’t mean only health regulations, but also the broader laws that surround introducing any product or service. Innovators will want to know whether they are at risk of breaking a rule, and how the risks of liability are distributed.
IC: In the current health system, the decision-making process relies heavily on the experience and expertise of doctors. In a world where artificial intelligence (AI) helps make decisions, can we expect the roles of doctors to change?
FR: Doctors are evolving for the better. Those who do not embrace this new technology are in danger of not being on the cutting edge of new healthcare treatments and discoveries. The new generation of doctors will be successful if they can merge traditional medical skill sets with data management skills. The doctor who will help the public and their future patients will be that hybrid of data manager and thoughtful listener. These are the doctors where I focus my teaching now — they are the future.
EW: From the research we have been doing on the future of work and artificial intelligence, it seems that machines could do some of the tasks that doctors do, but not replace the role — which instead could grow and change. Ideally, we could use technology to get a handle on wait times and bottlenecks in medical diagnosis and treatment, especially as the population ages. Personally, I hope that new tools enable more collaboration among doctors, nurses, physiotherapists, dieticians, social workers, mental health professionals, and other partners to focus on the health of each person in the broader context of their life.

Is there a limit to the human lifespan?
IC: What do all of these innovations in healthcare imply for aging? For example: Will people be expected to work longer if they live longer? What does this mean for life/health insurance? Could people live to meet their great-great-great grandchildren?
FR: The simple answer is yes. People are going to live longer, especially as cures for more cancers and chronic illnesses — such as inflammatory diseases — become available. However, with patient longevity comes a societal impact that government bodies will need to address. There is potential for other healthcare consequences to surface that put significant pressure on the healthcare system (e.g. additional care for extending lives). We need mechanisms in place to ensure that a healthier population can enjoy a good quality of life.
EW: Maybe ask me again in another 100 years (laughs).
With antimicrobial resistance, global income inequality, and other threats to human health, I don’t think we can rest on our laurels and expect an inevitable large boost in average lifespan. The science of aging may produce breakthroughs, but there is a lot more going on.
In the event that healthy lifespan does increase greatly, we’ll obviously have to look at how retirement, pensions, and social supports will work. My personal hope is that we would put a lot of that additional time into supporting young families and creating great conditions for child development. That might involve sequencing education, career, and child-raising differently. Maybe it would also involve creating more opportunities for people of all ages to contribute directly to raising the next generations. I would be delighted if the time and wisdom acquired with longer life was also directed at restoring degraded and threatened ecosystems.
For updates, interesting science, questions and/or comments please reach out to @PolicyHorizons and/or @imagia_ai
Please note: this interview has been edited for length and clarity.